Dispelling the Myth Around Imaging and Back Pain
If you’ve had back pain, you’ve likely considered getting an image - either an x-ray, MRI, or CT scan. I’ve had a lot of my clients come into the clinic bringing their imaging in great despair. They say things like:
“Look at this report - my back is messed up”
“My doctor says I have spinal stenosis - I guess there’s no hope for me”
“My discs are bulged - is that even fixable?”
“I have disc degeneration - what does that mean?”
“I’ll definitely need surgery in the future”
“My body’s a mess, just put me out to pasture”
I’ve seen medical imaging produce fear in people which has prompted me to write this blog for our clients and anyone else suffering through back pain. Reading certain words can create fear resulting in paralysis by analysis. This results in failure to seek help because people feel hopeless.
I’m here to tell you that your image does not define your outcome and that it is only a piece of the puzzle when it comes to injuries.
Do I need an image before seeing a physiotherapist?
Though an image is a great piece of information, this is not true. An image doesn’t explain why you have pain. There are so many other factors that affect pain and on top of that, a diagnostic image only represents what your spine looks like when you are stationary. It does not provide understanding around why it hurts when you move.
Consider this, when you get an MRI, the position you are lying in is flat on your back with your legs straight. It is not an image when you are:
Bending to pick something up off the ground
Carrying your son or daughter
Taking clothes out the laundry
Taking your dog for a walk
Lifting weights
Your body is a dynamic system. Thus, a static image of your spine will only present one piece of information. Some great questions that will help your physio determine what needs to happen next are:
What positions make your back worse?
What makes your back feel better?
Where does it hurt? Does your pain move?
Do you lose range of motion after a certain activity?
What have you tried so far?
The list goes on! Physiotherapists are great at listening to understand what your body needs to become pain free. We understand that pain is subjective - meaning it’s a personal experience that is unique to you. We want to hear your story and help you decipher what is making you sore.
Most Imaging Findings are Incidental
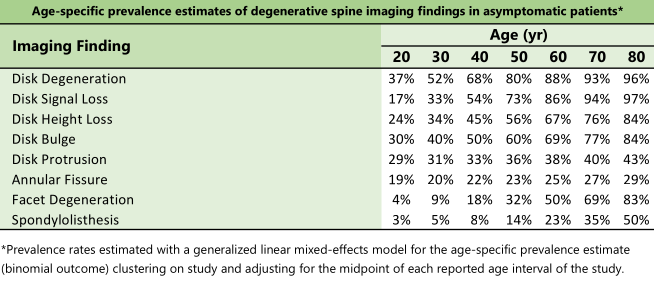
What you find on your medical image could have been there prior to your injury. This study looked at how often MRI and CT scan findings appear in people who do not have back pain¹. The findings assessed included:
Disc Degeneration
Disc Signal loss
Disc Height Loss
Disc Bulge
Disc Protrusion
Annular Fissure
Facet Degeneration
Spondylolisthesis
They found that in patients with no back pain, the above findings on MRI and CT scans become more common as you get older. In other words, you’d expect these findings to show up on your MRI and CT just like the fine wrinkles on your skin as you age.
When Imaging is Important
Imaging is helpful when there is strong indication for it. Your health care practitioner is trained to look for something known as a Red Flag🚩.
A Red Flag is a medical term describing a potentially serious issue that requires immediate attention. Here are some examples of red flags of the spine².
New trouble controlling your bladder or bowels. (accidents you can’t stop or difficulty going at all)
A sudden change in your ability to walk, balance or use of your hands for fine movements
Tingling, numbness or pain that travels down both arms or both legs
Tingling or numbness in the saddle region (the part of your body that would touch a bicycle seat)
Possible signs of infection or cancer in the spine (fever, chills and sudden severe back pain or unexplained weight loss)
A fall or minor accident in an older adult with osteoporosis (especially if they take steroid medication for a long time)
A previous lower back surgery with symptoms that are getting worse (increasing leg pain, weakness, numbness or tingling)
This list is not exhaustive and should not be used to determine whether you need imaging. Instead, it is best to talk to your physician or a physiotherapist trained to understand when it’s appropriate to order imaging. If something seems suspicious, your health-care professional will refer you to where you need to go.
All in all, if you have tried 6+ weeks of really good physio and exercise but there is no improvement and things are perhaps worsening - imaging might be warranted.
The Good, the Bad and Everything In-between
The good news is, you don’t always need medical imaging to start physiotherapy. Why is this good news? At the time of writing this blog, wait times in Canada for an MRI and CT are quite long. In Ontario the current average wait time for an MRI is 103 days for priority 4 patients.
Priority wha…?
In Ontario, people are placed in 4 different categories to make sure urgent cases are scanned first. Priority 4 means non-urgent and not time sensitive - not to say that your injury is not time sensitive. But the health care system is full of other people looking for answers as well. Below is a summary of this categorization.
Summary of Priority Categories for Imaging
| Priority 1 - Emergency | Rare - but someone who needs an immediate image because of sudden loss of function or trauma - they get scanned immediately. |
| Priority 2 - Urgent | A condition that needs attention soon, but not life threatening. Usually people who are in the hospital system already. |
| Priority 3 - Semi-Urgent | Your condition is stable, but your doctor probably wants an image sooner than later. |
| Priority 4 - Non-Urgent (most low back pain) | Your condition is stable and safe to wait. |
If you’re interested in looking for wait times in Ontario here is a link to the Ontario Health website for wait times around imaging, surgery and even breast screening wait times. https://www.ontariohealth.ca/system/reporting/wait-times
Cumulative Radiation Risk
Another upside to not getting imaging is limiting the amount of radiation absorbed by the body! Most people agree that they do not want to be exposed to any sort of radiation long term. By avoiding unnecessary imaging, you reduce the risk of its cumulative effects.
Here is one example I like to use when telling people about radiation exposure. A CT of the spine exposes your body to 6-10mSv of radiation (mSv -stands for millisievert - how much radiation your body absorbs).³ One lumbar x-ray exposes you to roughly 0.7mSv of radiation.⁴ That means you are getting 20-30 times more radiation exposure than just a single x-ray. We want to avoid any unnecessary imaging as the effects of imaging can add up!
Unfortunately, you’re still in a lot of pain and need a solution. Perhaps you were hoping the image would illuminate the reason for your pain and provide you the solution to being pain free.
Where do I start now?
In an effort to help my clients with lower back pain, I’ve written a lot of blogs about the experiences of my clients and my own personal journey with back pain. We are bombarded by too many options: chiro, massage, osteo, acupuncture, ultrasound, shockwave. We’re also inundated with large questions like:
Which medical image should I get?
What medications should I take?
Should I get surgery?
There are too many options and not enough guidance.
Everyone’s back pain is different. A trend I’m seeing are clients seeking help online through ChatGPT, Youtube, Instagram and Tiktok with minimal success. If it were a simple one-size-fits-all approach, most back pain would be gone. But it’s not, it's a complex phenomena with multiple factors at play.
70% of my caseload are clients with spinal injuries. Tingling, numbness, pins and needles, leg weakness and back pain that doesn’t change no matter what position they are in. Many of my clients are on pain medications and want to stop taking them because of the side effects. However, they are afraid to stop taking them because the pain is debilitating. The big question my back pain clients are most concerned about is whether they need surgery. They have heard a story from either a family member or friend who received surgery and the recovery time and risk that come with it.
Ultimately people want to be off medication and avoid surgery, but how can they do that if they are stuck in a constant loop of boom and bust with their recovery?
Our Approach
We begin by finding patterns with your pain. A conversation to help understand how you feel, what is limiting you, what makes you better or worse and how it’s affecting your life. These pieces of information will help us focus on the potential sources of your pain. We then use a repeated movement screen to see if the pattern you are reporting lines up with how your body moves. This is our way of confirming your history or changing course with constant reassessment each visit.
Your pain varies and requires an approach that is dynamic. Our approach changes with how your body is responding. No one-size-fits-all approach. We do not use the same method for each client, everything is tailored to your unique needs. We do not use a square peg for a round hole. Your body is unique and has unique needs that must be met.
I had back pain as well
I understand what it's like to have back pain. Tingling and numbness down my left leg constantly from a back injury 8 years ago. I couldn’t walk, couldn’t run, couldn’t enjoy life. It was terrible. I was depressed and didn’t know what to do. I sought help from 5 different clinicians and hours of research on the internet to find a solution. I now have a method that our team uses to see back pain from a different perspective. We understand what it’s like to have a back injury and we want to help you!
You’re in the lurch!
Basically no man’s land, you’re not a surgical candidate and your doctor is stumped. They tell you that “you just have to live with it.” This is not the answer you are seeking.
Our health care system is broken. But as a means to help those in the lurch, I’ve shared knowledge with my staff and the clients I’ve seen over 10 years of practice.
I understand what you are going through. It is tough to deal with the constant nagging and the stress that comes with a chronic injury. Our mission at Break Free is to help find solutions to help you recover and thrive. I wish that there was someone to help guide me what I was going through and so our goal is to become your guide through this mess.
If you’re interested in learning more about our approach to lower back pain, book with one of our physios today!
Low Back Pain Physiotherapy in London, Ontario
Looking for personalized help with low back pain or sciatica?
Learn more about our approach to low back pain physiotherapy in London, Ontario.
References
1. W. Brinjikji, P.H. Luetmer, B. Comstock, B.W. Bresnahan, L.E. Chen, R.A. Deyo, S. Halabi, J.A. Turner, A.L. Avins, K. James, J.T. Wald, D.F. Kallmes, J.G. Jarvik. Systematic Literature Review of Imaging Features of Spinal Degeneration in Asymptomatic Populations. American Journal of Neuroradiology Apr 2015, 36 (4) 811-816; DOI: 10.3174/ajnr.A4173
2. American College of Radiology. (2021). ACR Appropriateness Criteria®: Low Back Pain. ACR. https://acsearch.acr.org/docs/69483/narrative/
3. Brix, G., Lechel, U., Glatting, G., Ziegler, S. I., Münzing, W., Müller, S. P., & Beyer, T. (2005). Radiation exposure of patients undergoing whole-body dual-modality 18F-FDG PET/CT examinations. Journal of Nuclear Medicine, 46(4), 608–613.
4. Mettler, F. A., Jr., Huda, W., Yoshizumi, T. T., & Mahesh, M. (2008). Effective doses in radiology and diagnostic nuclear medicine: A catalog. Radiology, 248(1), 254–263.
Corey Kim
Physiotherapist
Hey, my name is Corey, and I’m a co-owner of Break Free Physiotherapy and Wellness. I was born in Seoul, South Korea but grew up in London, Ontario. I finished both my Bachelor of Arts in Kinesiology and Master of Physical Therapy degrees at Western University. I’m passionate about helping people find pain relief through movement and believe in self-empowerment by sharing knowledge of the human body and its ability to heal. [full bio]